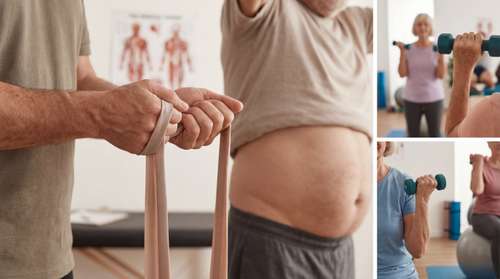
For decades, mainstream weight loss advice has focused almost entirely on the scale, treating every shed pound as a victory. But a groundbreaking study published on March 27, 2026, forces a radical shift in how we approach aging and wellness. Researchers have identified a dangerous physiological pairing known as sarcopenic obesity—the coexistence of low muscle mass and excess belly fat—that nearly doubles a person's risk of early death.
The findings expose a critical flaw in traditional diet culture, particularly for aging populations. When older adults lose weight without prioritizing muscle retention, they inadvertently invite a biological cascade that compromises their long-term survival. This revelation is accelerating the shift toward muscle-centric medicine, proving that preserving physical strength is just as vital as trimming waistlines.
The Science Behind the 83% Mortality Spike
The stark statistics driving today's headlines stem from extensive collaborative research led by the Federal University of São Carlos (UFSCar) in Brazil and University College London (UCL). Analyzing data from the esteemed English Longitudinal Study of Ageing, scientists tracked 5,440 participants aged 50 and older over a comprehensive 12-year period.
Their conclusion was unambiguous: individuals harboring both abdominal obesity and muscle loss faced an 83% higher death risk than those without either condition. The sheer magnitude of this belly fat death risk has prompted gerontologists to sound the alarm on how we monitor the health of older adults.
Interestingly, the data revealed that the dangers of a larger waistline are deeply tied to the amount of muscle beneath it. Participants who carried excess abdominal fat but maintained adequate muscle mass did not experience this severe mortality spike. Furthermore, those with low muscle mass but no abdominal obesity saw their mortality risk drop by 40% compared to the sarcopenic obesity group. The lethal threat lies not in either condition alone, but in their precise collision.
The Vicious Cycle of Inflammation and Muscle Breakdown
To understand why sarcopenic obesity acts as such a deadly duo, we have to look at the microscopic warfare happening inside the body. Excess abdominal fat does not just sit inertly around the organs; it acts as a highly active endocrine organ, constantly pumping out inflammatory cytokines into the bloodstream.
This systemic inflammation triggers widespread metabolic and catabolic changes that aggressively break down existing muscle tissue. The less active muscle tissue you have, the lower your resting metabolic rate drops. A sluggish metabolism inevitably promotes even more fat storage, creating a vicious cycle of abdominal obesity and muscle loss that accelerates the aging process and drives physical frailty.
Fat Infiltration: The Enemy Within
As the systemic inflammation persists, the dynamic between fat and muscle worsens. Fat begins to literally infiltrate the muscle tissue itself, taking up valuable space and degrading its structural integrity. This phenomenon compromises the muscle's metabolic, endocrine, and immunological capabilities. Instead of dense, powerful tissue capable of absorbing glucose and preventing falls, the muscle becomes marbled with fat, weak, and highly dysfunctional.
A Clinical Breakthrough for Early Detection
Historically, accurately diagnosing sarcopenic obesity posed a massive challenge. It generally required expensive, specialized equipment like MRI or CT scans, keeping proper diagnosis out of reach for routine medical care. Because it was so hard to measure, the condition often went unnoticed until a catastrophic health event occurred.
However, the March 2026 study proved that healthcare providers can now accurately screen for this dangerous combination using simple, highly accessible measurements. By measuring waist circumference and applying established equations that estimate lean mass based on routine clinical variables—such as age, sex, weight, and height—doctors can identify at-risk patients during a standard 15-minute checkup. Bypassing the need for costly imaging means millions of older adults can receive an early diagnosis, opening the door for timely, life-saving lifestyle interventions.
Rewriting the Rules of Fitness for Longevity
The undeniable link between muscle mass and longevity demands a complete overhaul of how we prescribe exercise to aging populations. For years, older adults were advised to take up walking, light aerobics, or gardening. While beneficial for cardiovascular health, these activities are no longer sufficient on their own to ward off physical decline.
The medical community is increasingly adopting a framework of muscle-centric medicine, emphasizing that skeletal muscle is the body's primary metabolic engine and an indispensable armor against chronic disease. To combat the onset of sarcopenic obesity, daily health protocols must aggressively integrate resistance exercises.
The Prescription: Strength Training for Seniors
Strength training for seniors is rapidly emerging as the ultimate preventative treatment. Lifting weights, utilizing resistance bands, and engaging in demanding bodyweight exercises actively rebuild the muscle fibers that systemic inflammation attempts to destroy. This type of training improves insulin sensitivity, fortifies bone density, and clears glucose from the blood.
Building a robust physical foundation prevents fat from monopolizing the body's internal real estate. As this latest research definitively proves, true fitness for longevity is not about starving yourself to reach an arbitrary target weight. It is about building resilient, highly functional muscle capable of sustaining you through the decades, ensuring your later years are defined by strength rather than fragility.