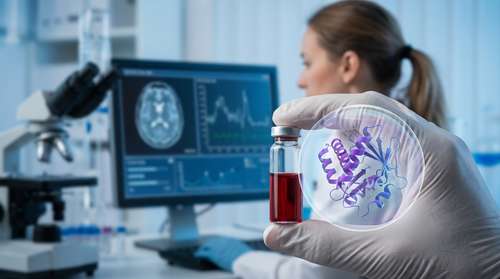
For decades, diagnosing neurodegenerative decline has been a race against the clock, often delivering answers only after irreversible damage has occurred. Now, a revolutionary advancement in early Alzheimer's detection is shifting the medical landscape. In a landmark study published in late February 2026, researchers have successfully demonstrated that tracking blood protein shape changes can accurately flag the disease years before memory loss or cognitive symptoms emerge.
The groundbreaking research, spearheaded by the Scripps Research Institute and detailed in the journal Nature Aging, introduces a fundamentally new way to evaluate neurological risk. Instead of merely measuring the quantity of specific biomarkers, scientists are now observing the physical "shape-shifting" of proteins circulating in the bloodstream. This novel approach is rapidly emerging as one of the most significant healthy aging breakthroughs of the decade, offering unprecedented hope for aging adults and clinical researchers alike.
The Science Behind Blood Protein Shape Changes
To understand why this method works, you have to look at how the human body maintains its cellular machinery. Healthy cells rely on a rigorous quality control system known as proteostasis to ensure proteins fold into their correct three-dimensional structures. When this system starts failing—a common precursor to neurodegeneration—proteins misfold, ultimately becoming toxic or non-functional.
The Scripps team hypothesized that if this folding system breaks down in the brain, the evidence would also appear in the blood. By analyzing plasma samples from 520 volunteers, the researchers identified three specific proteins that reliably indicate cognitive decline: C1QA (involved in immune signaling), Clusterin (linked to amyloid clearance), and Apolipoprotein B (which supports blood vessel health).
As the disease progresses, these proteins literally change shape, becoming less structurally "open" and more closed off. Tracking these specific alterations allowed the researchers to distinguish healthy individuals from those with Mild Cognitive Impairment (MCI) with an astonishing 93% accuracy. This makes the test a powerful tool for early Alzheimer's detection.
Why Shape-Shifting Outperforms Traditional Alzheimer's Blood Biomarkers
Current diagnostic methods largely rely on measuring the concentrations of amyloid beta and phosphorylated tau (p-tau) in the blood or spinal fluid. While these Alzheimer's blood biomarkers are valuable, they often reflect late-stage biological shifts. Protein concentration fluctuates for various reasons, but structural folding errors act as a direct, early warning signal of cellular stress.
Using a sophisticated technique called covalent protein profiling combined with artificial intelligence and mass spectrometry, the researchers mapped out exactly which parts of the protein surface were exposed or buried. "The correlation was amazing," noted Casimir Bamberger, a senior scientist at Scripps Research. Finding three distinct sites on three different proteins that synced so perfectly with disease progression was an unexpected and powerful validation of the model.
Uncovering Genetic and Gender Differences
Beyond simple detection, looking at blood protein shape changes offers a much deeper look into the biology of dementia. The researchers found that structural markers correlated with known genetic risk factors, such as the APOE ε4 variant. Furthermore, analyzing protein folding helped highlight distinct differences in how neuropsychiatric symptoms present between men and women—nuances completely invisible to traditional Alzheimer's blood biomarkers.
Tracking Disease Progression in Real-Time
What makes this testing mechanism exceptionally practical is its longitudinal reliability. When researchers tested follow-up blood samples months later, the structural panel correctly tracked disease progression 86% of the time. The scores from this test also strongly correlated with clinical cognitive exams and moderate brain shrinkage observed via MRI scans.
A Major Leap for Preventative Brain Health
The clinical implications of this test extend far beyond a simple diagnosis. Catching the breakdown of proteostasis before irreversible amyloid plaques accumulate gives medical professionals a crucial head start. According to Dr. Richard Hodes, director of the NIH's National Institute on Aging, this introduces a "fundamentally new, blood-based approach" that captures biological features completely missed by existing diagnostics.
For patients prioritizing preventative brain health, this type of predictive screening could soon become a cornerstone of routine medical care. If physicians can identify those at risk during the earliest molecular stages, patients might benefit immensely from emerging therapeutic interventions before significant neural networking is lost. For instance, tracking protein structures could verify whether new neuroprotective drugs are actively helping proteins return to their healthy, "open" shapes.
What This Means for Dementia Screening 2026 and Beyond
As we navigate the future of longevity diagnostics, the shift from measuring "how much" to "what shape" represents a massive leap forward. While the test requires further validation in larger, more diverse patient populations before it arrives at your local doctor's office, the scientific foundation is undeniably set.
The reality of routine dementia screening 2026 is looking increasingly non-invasive, precise, and proactive. By examining the exact structural architecture of our blood, the latest healthy aging breakthroughs are finally giving us a fighting chance to intercept Alzheimer's disease before it claims our most precious memories.