For decades, the conversation surrounding modern diets has focused predominantly on waistlines and body mass index (BMI). But a landmark investigation published on April 14, 2026, in the journal Radiology has completely reframed how we view nutritional health. Researchers have uncovered a startling connection between ultra-processed foods and muscle aging, revealing that highly processed diets directly cause fat to infiltrate muscle tissue—even in people who appear perfectly healthy on the outside.
This condition, known medically as myosteatosis, acts as a silent thief of physical independence. By replacing dense, functional muscle fibers with streaks of fat, the empty calories from ultra-processed diets are fast-tracking structural decline and joint deterioration. The study proves that looking thin is no longer an accurate measure of musculoskeletal health.
Unpacking the Muscle Quality MRI Study
Led by Dr. Zehra Akkaya at the University of California, San Francisco, this groundbreaking muscle quality MRI study provides definitive evidence of the link between ultra-processed foods and muscle aging. Researchers analyzed 615 men and women with an average age of 60. All participants were part of the Osteoarthritis Initiative, a nationwide research program sponsored by the National Institutes of Health designed to track and prevent skeletal decline.
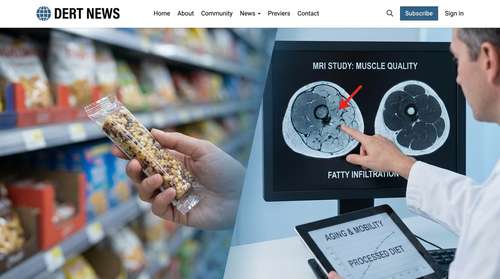
Researchers utilized non-enhanced MRI scans and the Goutallier grading system to evaluate thigh muscle composition, specifically targeting the adductors, flexors, and extensors. They combined this imaging data with detailed food frequency questionnaires. The dietary analysis revealed that, on average, a staggering 41% of the food consumed by participants over the previous year was ultra-processed.
The results were unequivocal. Individuals who consumed higher amounts of these engineered foods exhibited significantly greater fat infiltration within their thigh muscles. Strikingly, this severe structural degradation occurred regardless of the total calories the participants ate, their physical activity levels, or their baseline BMI.
What Drives Myosteatosis in Seniors?
Why do modern convenience foods wreak such havoc on human tissue? Products like mass-produced bread, packaged snacks, sugary cereals, and frozen meals are stripped of their natural matrices and loaded with artificial additives, emulsifiers, and refined carbohydrates. While these foods trigger the brain's reward system and provide immediate, cheap energy, they lack the essential amino acids and micronutrients required to maintain lean tissue mass.
Over time, this chronic nutritional deficit combined with systemic inflammation forces the body into a state of metabolic dysfunction. Fat cells begin to accumulate inside the muscle fibers themselves—a classic hallmark of myosteatosis in seniors. This intramuscular marbling compromises physical strength and acts as one of the primary sarcobesity risk factors. Sarcobesity, the dangerous combination of low muscle mass and high visceral or intramuscular fat, is notoriously difficult to reverse. It exponentially increases the likelihood of metabolic diseases like type 2 diabetes and leads to severe mobility impairment.
A Critical Factor in Knee Osteoarthritis Prevention
One of the most alarming aspects of fatty muscle infiltration is its immediate, mechanical impact on joint health. The thigh muscles serve as the primary shock absorbers and dynamic stabilizers for the knee. When these muscles become marbled with fat, they lose their tensile strength and fail to brace the joint properly during movement.
As a result, the physical burden of walking, climbing stairs, and standing shifts directly onto the cartilage and bones. The Radiology study highlighted that deteriorating muscle quality accelerates the onset of joint degradation, making dietary intervention a non-negotiable pillar of knee osteoarthritis prevention. Medical professionals now urge patients to realize that alleviating joint pain requires more than just traditional weight loss; it requires completely overhauling the source of their calories to restore tissue integrity.
The Blueprint for a Healthy Aging Diet 2026
Because the tissue damage from ultra-processed foods operates independently of simple calorie counting, traditional weight loss regimens that merely restrict food intake are fundamentally flawed. If you want to protect your skeletal integrity, adopting a healthy aging diet 2026 plan means focusing relentlessly on food quality.
- Prioritize Whole Proteins: Ensure adequate intake of lean meats, fish, eggs, and legumes to provide the amino acids necessary for muscle repair.
- Eliminate Industrial Additives: Swap out pre-packaged convenience items for meals cooked from scratch using single-ingredient whole foods.
- Focus on Anti-Inflammatory Fats: Incorporate omega-3 fatty acids found in walnuts, flaxseeds, and salmon to help combat the systemic inflammation triggered by heavy UPF consumption.
A New Standard for Preserving Mobility in Elderly Populations
The traditional reliance on the bathroom scale to measure health is rapidly becoming obsolete. As advanced imaging technology becomes more integrated into preventative care, the medical community is recognizing that true physical vitality lies in tissue quality.
Understanding the connection between ultra-processed foods and muscle aging is the first step toward better health. Preserving mobility in elderly populations starts at the grocery store, well before the first signs of joint pain or muscle weakness appear. By decisively cutting ultra-processed foods from our daily routines, we can halt the progression of fatty muscle disease, safeguard our weight-bearing joints, and secure our physical independence for decades to come.