For decades, Alzheimer's disease has been a silent thief, quietly altering the brain long before the first missed appointment or forgotten name. By the time memory loss becomes undeniable, significant neurological damage has already occurred. But what if you could foresee your cognitive future decades before the symptoms surfaced? A revolutionary Alzheimer's blood test is making this a reality. According to a landmark study published this week in JAMA Network Open, measuring a specific biomarker can accurately forecast dementia risk up to 25 years in advance. This unprecedented window of opportunity is redefining healthy aging 2026 and shifting the paradigm from reaction to true prevention.
The Breakthrough in Early Dementia Detection
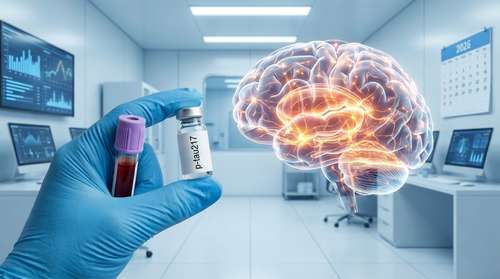
The mechanics behind this diagnostic leap focus on a protein known as phosphorylated tau 217, or p-tau217. In a healthy brain, tau proteins help stabilize the internal scaffolding of nerve cells. However, when Alzheimer's disease begins to take root, these proteins misfold and clump together, forming toxic tangles that disrupt cellular communication. These microscopic changes initiate a slow biological cascade that eventually destroys memory and cognition. The recent study tracked 2,766 cognitively healthy older women who participated in the Women's Health Initiative Memory Study. Over a remarkable 25-year follow-up period, researchers analyzed their baseline blood samples to measure these circulating tau proteins. The findings offer a stunning glimpse into the future of neurological care.
How p-tau217 Dementia Screening Works
The results from the University of California San Diego research team were staggering. Women who exhibited the highest levels of p-tau217 in their bloodstream at the study's onset were significantly more likely to develop mild cognitive impairment or dementia later in life. In fact, elevated baseline levels corresponded to a threefold higher hazard of developing all-cause dementia compared to those with lower levels. Unlike expensive PET scans or invasive lumbar punctures, this simple p-tau217 dementia screening captures the silent biological buildup of the disease with remarkable accuracy. It provides a dynamic picture of risk, allowing physicians to detect molecular warning signs long before subjective cognitive decline becomes evident to the patient or their family.
Unpacking the Data: Who Is Most at Risk?
While the predictive power of this biomarker is a massive leap forward for senior wellness news, researchers emphasize that the risk profile is not uniform across all demographics. Lead study author Dr. Aladdin H. Shadyab and his colleagues found that the association between high p-tau217 and future cognitive decline was particularly strong among specific groups. White women, individuals over the age of 70, and those carrying the APOE e4 genetic variant—widely recognized as the strongest genetic risk factor for late-onset Alzheimer's—demonstrated an even sharper correlation with future impairment. Interestingly, the study also revealed a stronger link among women who utilized estrogen plus progestin hormone replacement therapy compared to those taking a placebo. These crucial nuances highlight the importance of personalized medicine when interpreting brain health markers, reminding us that genetics, age, and medications all interact to influence our cognitive destiny.
Brain Health Prevention: Why an Early Warning Matters
You might naturally wonder why anyone would want to know their dementia risk decades in advance, especially if a definitive, overarching cure does not yet exist. The answer lies in the immense power of time. Having a 25-year lead time is arguably one of the most significant longevity breakthroughs in modern neurology. It provides a massive, actionable runway for proactive brain health prevention. When memory problems are finally diagnosed in a clinical setting, doctors are often attempting to salvage a brain that has been under attack for twenty years. By shifting the timeline, we can implement protective strategies when the brain is still highly resilient and fully functional.
Actionable Steps for Healthy Aging 2026
When armed with the knowledge of elevated risk, patients can adopt rigorous, evidence-based lifestyle modifications that drastically alter their trajectory. Interventions such as optimizing deep sleep architecture, managing chronic stress, engaging in intensive cardiovascular exercise, and maintaining high social and cognitive engagement have all been shown to support neurological resilience. Furthermore, identifying high-risk individuals early fundamentally changes how we approach medical research. It accelerates clinical trials, helping pharmaceutical companies test preventative drugs before irreversible brain damage occurs. Participants can enroll in studies targeting amyloid and tau clearance at the precise moment those therapies are most likely to succeed.
The Future of Clinical Care and Cognitive Longevity
As we process this exciting development, it is important to contextualize what this Alzheimer's blood test actually means for the average person. Medical experts caution that an elevated p-tau217 result is an indicator of statistical risk, not a definitive diagnosis. Having higher levels means you are more likely to develop the condition than someone with lower levels, but it does not absolutely guarantee a future of dementia. Currently, these advanced blood-based biomarkers are primarily utilized in clinical trials and specialized research settings rather than routine annual physicals for asymptomatic adults. However, as the science matures and the testing infrastructure scales, routine early dementia detection will likely become a standard tool in primary care. Until that day arrives, this research serves as a powerful reminder that the foundation for sharp cognition in your eighties is actively built during your fifties and sixties. The era of passively waiting for memory loss to strike is officially over; the future belongs to proactive, lifelong cognitive care.